
Pain – Understanding the Mechanisms & How to Manage It in Sports
Introduction
Pain is one of the strongest signals the body sends to the brain to indicate that something is wrong. However, pain does not always mean serious tissue damage. In sports medicine and injury rehabilitation, understanding the mechanisms of pain helps athletes and coaches develop appropriate training adjustments and treatment strategies, avoiding both excessive rest and training beyond safe limits.
1. What is Pain?
According to the International Association for the Study of Pain (IASP), pain is “an unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage.” This means:
Pain is not just a physical signal; it is influenced by psychological, emotional, and contextual factors.
Two people with the same injury may experience very different levels of pain.
“Pain is weird.” — Paul Ingraham
“Pain can happen even when nothing is wrong, and pain can be absent even when something is wrong.” — Paul Ingraham
About the author: Paul Ingraham is a Canadian medical science journalist specializing in pain science, musculoskeletal conditions, and injury rehabilitation. He founded PainScience.com, a globally respected site for explaining complex physiology and medical research in an accessible, evidence-based way.
These quotes highlight:
Pain does not always reflect real tissue damage. For example, central sensitization can cause the brain to generate pain even when tissues are no longer injured.
Conversely, injury may exist without pain. This often occurs when the body releases adrenaline or endorphins during stress, competition, or survival situations, temporarily masking pain signals.
This reminds us that pain perception alone should not determine assessment; clinical evaluation, imaging, and monitoring of movement function are essential for informed decisions.
2. The Physiological Mechanism of Pain
2.1. Pain Detection (Nociception)
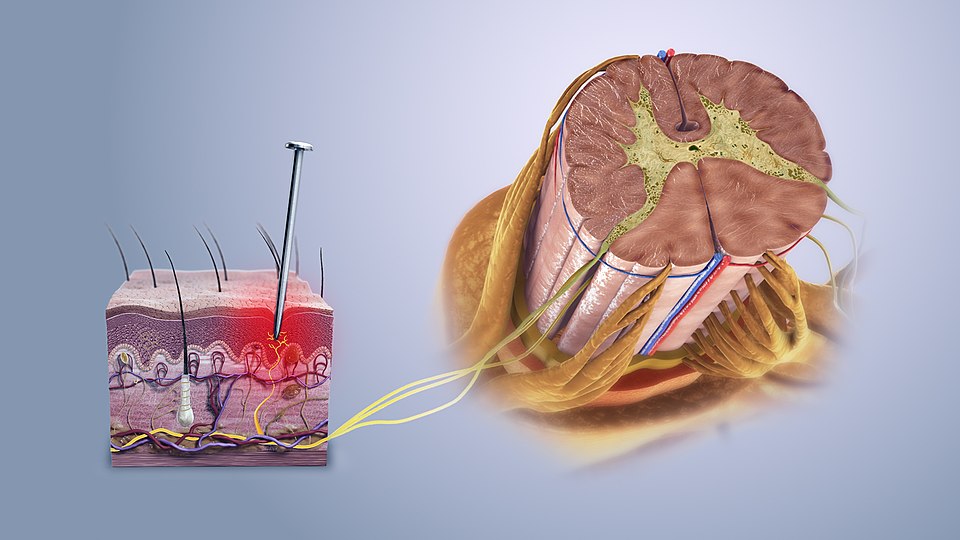
Nociception is the process of detecting harmful stimuli in the skin, muscles, tendons, or joints and sending signals to the spinal cord.
Illustration: When the skin is pricked by a sharp object, signals travel via sensory nerve fibers to the spinal cord and then to the brain. (Source: Wikipedia)
Nociceptors in the skin, muscles, tendons, and joints are activated when tissue is damaged.
Chemicals like prostaglandins, bradykinin, and histamine are released, increasing nociceptor sensitivity.
2.2. Signal Transmission
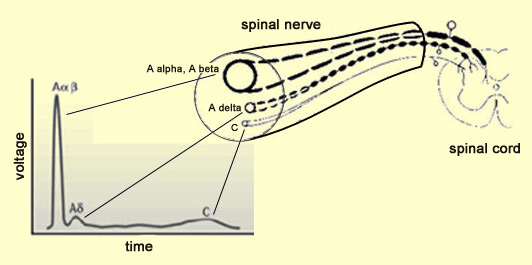
Sensory nerve fiber types — Aα, Aβ, Aδ, and C fibers, with conduction speed and roles in pain perception. Source: Thebrain.mcgill.ca
Once nociceptors are activated beyond a threshold, electrical impulses are generated.
These impulses travel via A-delta fibers (fast, sharp pain) and C fibers (slow, dull pain) to the spinal cord.
The spinal cord performs preliminary processing and sends signals to the brain. The brain does not send “pain signals” outward; it receives peripheral information and modulates the perception of pain.
2.3. Perception and Modulation
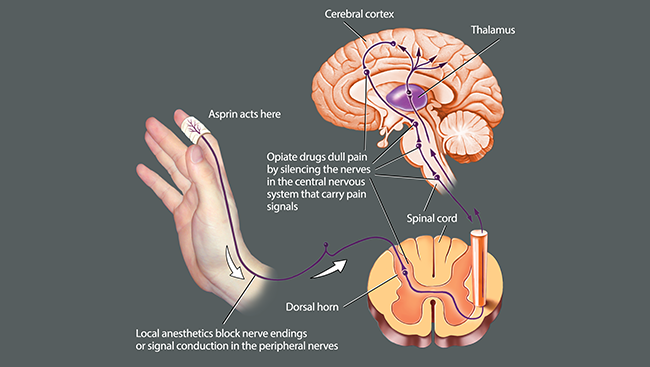
How the brain processes pain signals, interacting with tissues, the environment, and the central nervous system. Source: sfn.org
Brain regions such as the thalamus, somatosensory cortex, and limbic system analyze intensity, location, and associated emotions.
The brain can amplify or dampen pain perception through endogenous pain inhibition systems (endorphins, serotonin).
3. Types of Pain
Acute pain: Sudden onset, usually due to injury or inflammation. Serves a protective role, forcing rest.
Chronic pain: Lasting >3 months, often linked to nervous system changes and altered pain processing (central sensitization).
Referred pain: Felt in a location different from the actual tissue damage (e.g., left shoulder pain from a heart problem).
4. Factors Affecting Pain Perception
Psychological: Anxiety and stress can intensify pain.
Experience: Prior injuries can alter perception.
Environment: Sports competition or performance pressure can affect how the brain processes pain.
Biological factors: Gender, genetics, and hormones (estrogen, testosterone) play a role.
5. Applying Pain Understanding in Sports
Not all pain requires complete rest. Some delayed-onset muscle soreness (DOMS) is a normal adaptation.
Acute, worsening pain or pain with swelling/functional loss requires medical assessment.
Adjustment strategies include reducing load, modifying technique, and using supportive therapies (cryotherapy, heat, massage, EMS, red light therapy, etc.).
6. Pain Management and Relief Strategies

Physical strategies: Cold or heat therapy, compression, limb elevation, stretching, massage.
Active strategies: Active recovery, adjusting training volume, refining movement technique.
Psychological strategies: Breathing techniques, meditation, cognitive-behavioral therapy (CBT).
Nutrition: Omega-3 fatty acids and polyphenol-rich foods (berries, green tea) help reduce inflammation.
Conclusion
Pain is a complex phenomenon influenced by physiology, psychology, and context. Understanding its mechanisms and types helps distinguish “good” pain (adaptive) from “bad” pain (warning of danger). In sports, scientifically managing pain supports sustained performance and long-term health.